What is a Root Canal Infection?
A root canal infection happens when bacteria enter the inner part of a tooth, called the pulp. The pulp contains the tooth’s nerve and blood supply. Once bacteria reach this area, the nerve becomes inflamed and eventually infected.
This condition can be extremely painful and often requires urgent dental care. Without treatment, a root canal infection can spread to the surrounding bone, gums, or even the face.

What Causes a Root Canal Infection?
Several factors can lead to a root canal infection, including:
Untreated tooth decay
Cavities that are left untreated can deepen, allowing bacteria to reach the pulp.
Broken or chipped teeth
Exposed tooth structure creates a pathway for bacteria to enter.
Dental trauma
An accident or injury can damage the nerve, causing it to die and become infected.
Previous dental work
Cracked teeth
Cracks act as “highways” (pathway) for bacteria to reach the pulp.
Severe gum disease (periodontitis)
Infection can spread from the gums into the roots of teeth.
Signs and Symptoms of a Root Canal Infection
Pain is a common sign of a root canal infection, but it is not always reliable. Once the nerve dies, the tooth itself may not feel painful — instead, the surrounding tissues and bone become inflamed.
Common symptoms include:
- Severe, throbbing toothache that painkillers cannot relieve
- Swelling along the gumline or jaw near the infected tooth
- Facial swelling if the infection spreads
- Pain that disturbs sleep, often worse at night
- Extreme sensitivity to hot and cold foods or drinks
- Pain on chewing or biting
- Darkened or discoloured tooth (a sign of nerve death)
- Dental abscess – pus-filled swelling around the tooth root
If you notice these symptoms, it is important to see your dentist quickly before the infection worsens.

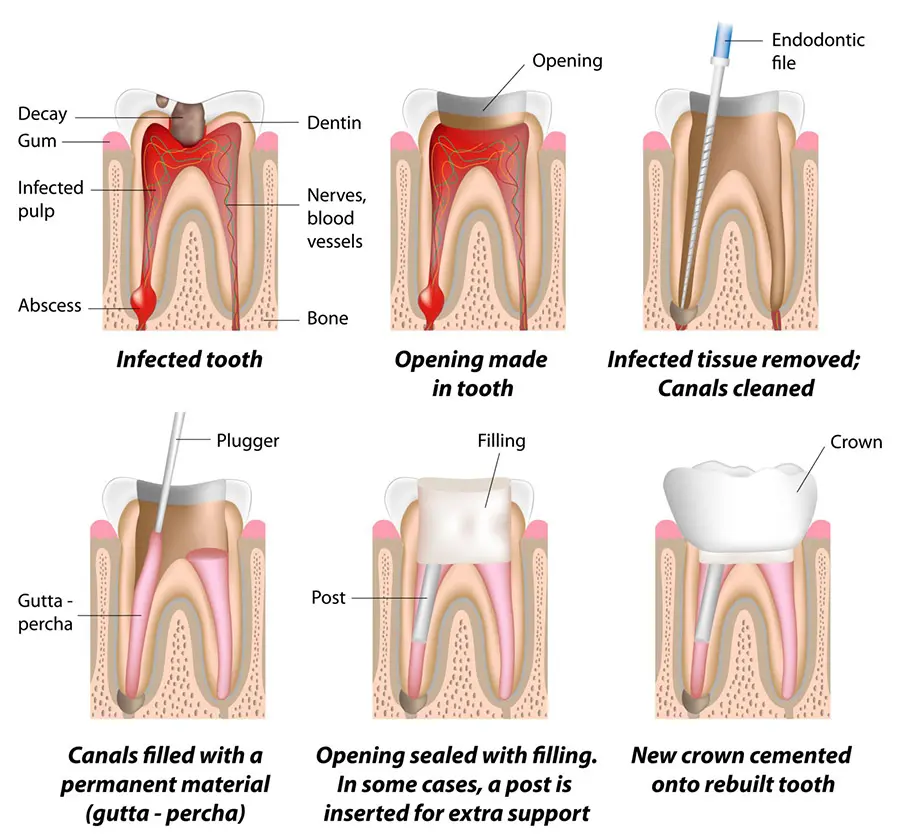
How is a Root Canal Infection Treated?
There are two main options for treating a root canal infection:
Root Canal Treatment (RCT)
This is a specialist procedure to save the tooth. It involves:
- Removing the infected pulp and nerve tissue
- Cleaning and disinfecting the root canal system with specialised instruments
- Filling the space inside the tooth with a protective material
- Restoring the tooth with a crown or onlay to strengthen it
When performed successfully, root canal treatment allows you to keep your natural tooth and restore full function.
Tooth Extraction
In cases where the tooth cannot be saved, extraction may be recommended. Removing the infected tooth eliminates the source of infection and allows the area to heal. After extraction, replacement options such as implants, bridges or dentures can be considered if required
Additional Treatments
- Drainage may be required if there is facial swelling or an abscess.
- Periodontal treatment may be necessary if gum disease is also present.
Preventing a Root Canal Infection
The best way to prevent a root canal infection is through early detection and regular dental care. Prevention tips include:
- Regular dental check-ups – Early detection allows small cavities to be treated before they reach the nerve.
- Routine dental X-rays – Help detect hidden decay and early signs of infection.
- Professional cleaning – Removes tartar and reduces the risk of gum disease.
- Good oral hygiene – Brush twice daily with fluoride toothpaste and floss daily.
- Healthy diet – Limit sugary snacks and drinks that feed bacteria.
- Seek help early – If you feel pain, sensitivity, or something unusual in your mouth, don’t wait for it to get worse.
Delaying treatment often means more complex and costly procedures later.
Book in to see our Expert Dentist for your infected root canal assessment today!
Dental Services
Full Mouth Dental Implants
Dental Implants
Invisalign
Clear Aligners
Cosmetic Dentist
Veneers
Sleep Dentistry
Teeth Whitening
Wisdom Tooth
Orthodontics
Jaw Expansion
Tooth Extraction
Dental Crown
Dental Bridge
Root Canal Treatment
General Dentistry
Gum Disease Treatment
Tooth Filling
Teeth Cleaning
Dentures
Sleep Apnoea
TMJ
Occlusal Splint
Mouth Guard
Family Dental
Kids Dental
Silver Diamine Fluoride
Fissure Sealants
Frequently Asked Questions

What is the most common cause of jaw pain?
The most common cause is bruxism (teeth grinding or clenching), often linked with stress, sleep apnoea, or misaligned teeth. It puts excess pressure on the jaw joint and surrounding muscles, leading to pain and stiffness.
Can jaw pain cause headaches?
Yes. TMJ disorders are closely linked with tension headaches and migraines because tight jaw muscles can radiate pain to the head, neck, and shoulders.
How do I know if my jaw pain is serious?
If you experience persistent pain, jaw locking, difficulty chewing, or worsening symptoms, it may indicate a serious TMJ disorder or another medical condition that needs immediate professional assessment.
Can stress cause jaw pain?
Absolutely. Stress is a major trigger for clenching and grinding, which strains the jaw joint and muscles. Learning relaxation techniques and wearing a nightguard can help.
What is the best treatment for jaw pain?
The best treatment depends on the cause. Nightguards, physiotherapy, jaw exercises, and stress management are highly effective. Severe cases may need dental correction or, rarely, surgery.